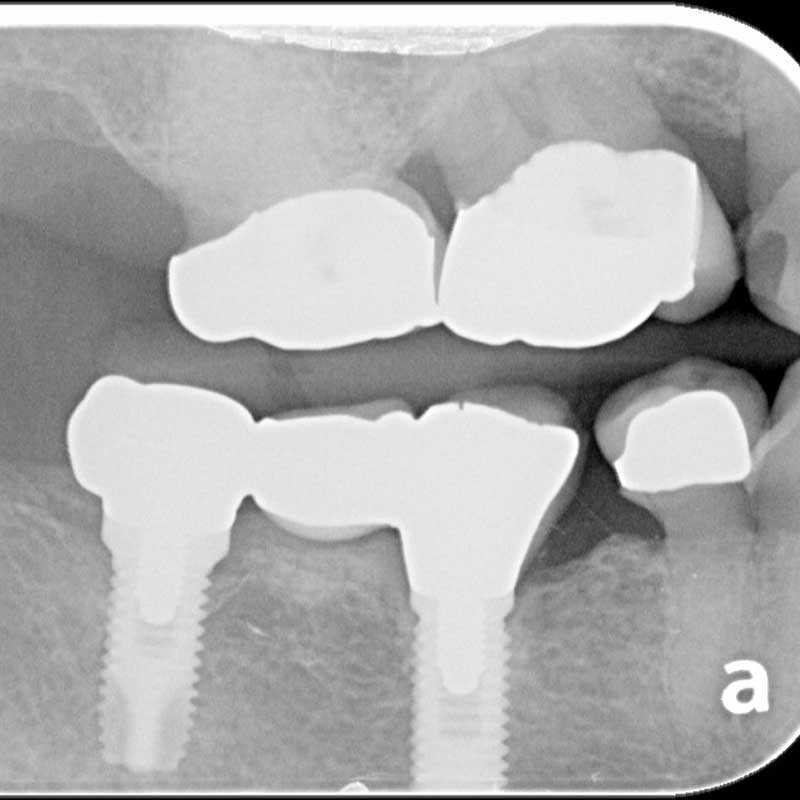
Sub-Pontic Osseous Hyperplasia
Subpontic osseous hyperplasia (SPOH) refers to the abnormal, excessive growth of bone tissue beneath the pontic of a fixed dental prosthesis or “bridge”. This is a rare but significant condition that can arise in patients with fixed dental prostheses (FDPs) replacing missing teeth. This condition can occur with both tooth-supported and implant-supported FDPs. Though often asymptomatic and discovered incidentally during routine radiographs, SPOH can lead to functional issues and complicate prosthetic rehabilitation. This article is intended to bring awareness to SPOH, emphasizing its etiology, diagnostic approach, clinical presentation, and management options.
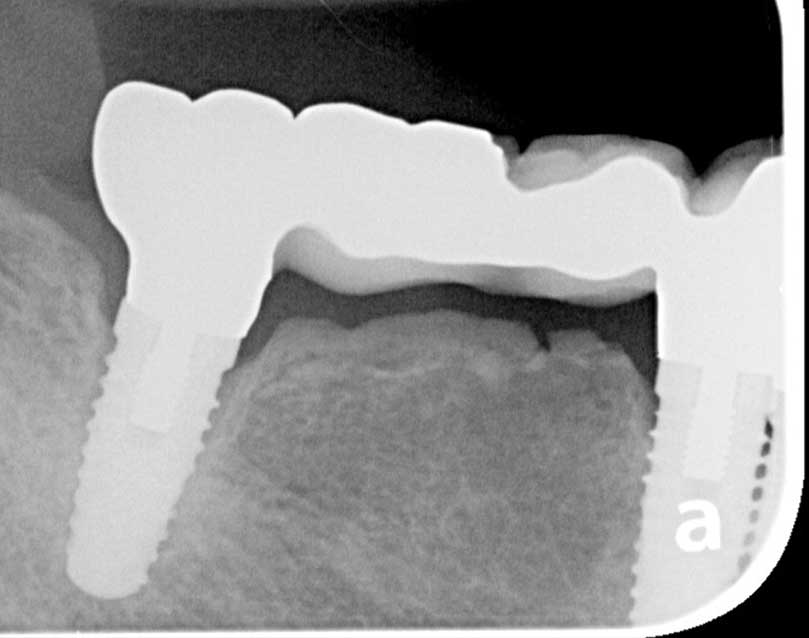
Case #1: Platform matched external-hex implants. Still convinced this causes bone loss?
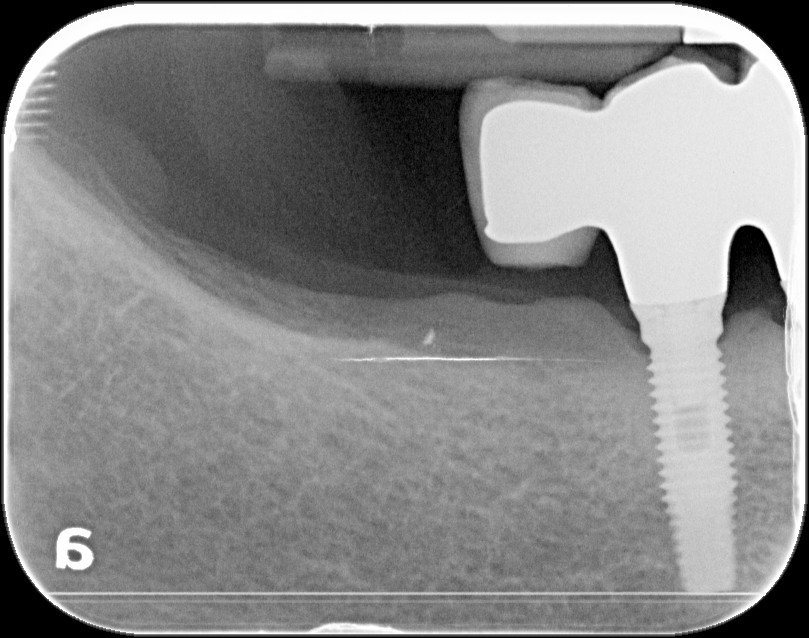
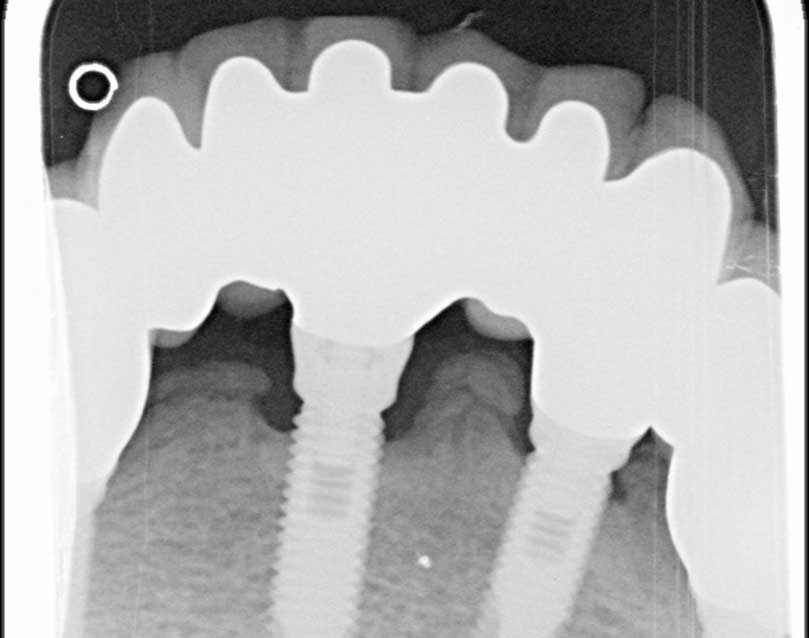
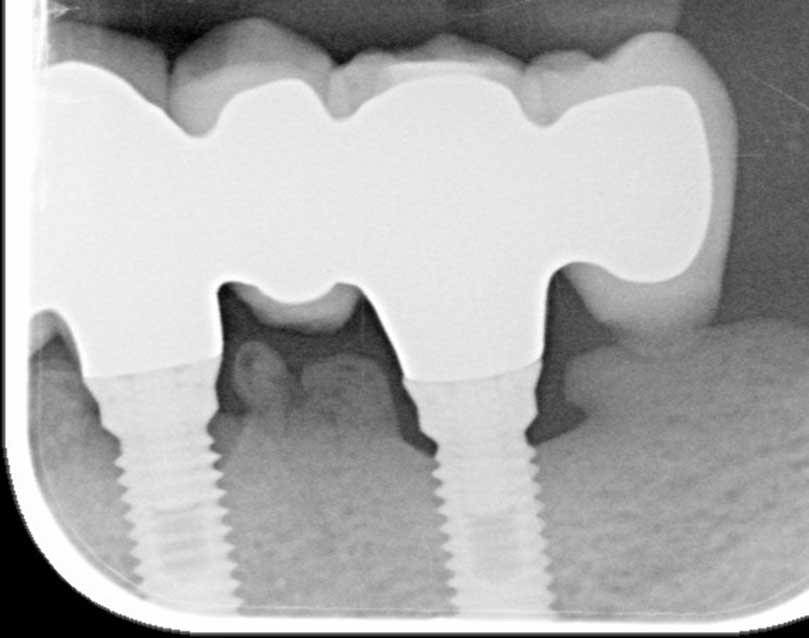
Etiology and Pathophysiology of SPOH
Though the precise cause of SPOH is still not fully understood, several key mechanisms have been suggested. My clinical experience has been that it is not possible to predict which of your patients will develop SPOH, but I do seem to appreciate this more in patients that exhibit increased occlusal loading from bruxism and clenching. It is my opinion that the current dental literature has not investigated this condition thoroughly enough to be more predictive. Below are the mechanisms that have been suggested in the available scientific literature.
Mechanical Stimulation from the Pontic
The most widely accepted theory behind SPOH involves mechanical stimulation. A fixed partial denture can create localized pressure on the alveolar ridge and underlying bone. This pressure can cause remodeling of the bone, potentially leading to excessive bone formation in the subpontic area.
Occlusal Forces and Functional Load
During normal chewing and functional movements, forces transmitted through the dental prosthesis to the underlying alveolar bone can encourage osseous changes.
Inflammatory Response
Chronic irritation or minor inflammation from improperly designed pontics, or from plaque accumulation around the bridge, could also trigger bone growth. Inflammatory cytokines released during this process may stimulate osteoblasts (bone-forming cells) in the affected area, leading to hyperplasia.
Inadequate Prophylactic Measures
Inadequate oral hygiene and inadequate maintenance of the prosthesis are risk factors for developing SPOH. The accumulation of biofilm around the pontic, which can lead to chronic gingival irritation, may indirectly promote bone changes. Routine maintenance and oral hygiene practices are critical in preventing such complications.
Clinical Presentation of SPOH
Most cases of subpontic osseous hyperplasia are asymptomatic, discovered incidentally during routine radiographic examinations. However, clinical signs and symptoms can occasionally arise, particularly in more advanced cases. Some can be severe enough to cause pain and discomfort, but this is usually self-limiting requiring no treatment.
Radiographic Signs: SPOH typically presents as an increased radiopacity beneath the pontic. In the early stages, it may appear as a subtle, localized increase of bone density. As the condition progresses, the bone growth can become more pronounced, potentially affecting the fit of the bridge or interfering with occlusion.
Functional Impairment: In cases where significant bone growth occurs, the pontic may come into more contact with the underlying residual ridge than was initially the case at time of the restoration placement. The patient may report discomfort or difficulty with oral hygiene or mastication in the area.
Occasional Pain or Discomfort: While most cases are asymptomatic, some patients may experience pain or a sense of pressure, particularly if the excess bone growth puts stress on the surrounding tissues or disrupts the fit of the bridge.
Osseous necrosis and localized infection: Occasionally the pressure can become severe enough to restrict blood supply and result in necrotic osseous sequestra that become infected and need to be removed.
Diagnosis of SPOH
Diagnosis of subpontic osseous hyperplasia is usually made through routine radiographic examination, with the condition appearing as localized bone growth beneath the pontic. However, distinguishing SPOH from other conditions is essential to avoid misdiagnosis.
Radiographic Evaluation
- Periapical Radiographs: These provide a more detailed image of the area beneath the pontic, revealing bone growth often as an increased radiopacity and increased vertical height closing the space to reach the intaglio surface of the pontic. A well-circumscribed area of bone density is typical, but variations in size and shape should be assessed.
- Panoramic Radiographs: While not as detailed, panoramic radiographs can offer a broader view of the edentulous areas and surrounding structures. A well-defined radiopaque area under the pontic can be a diagnostic clue.
- CBCT: Not typically as helpful due to the beam hardening and radiographic artifacts typically seen with this imaging modality.
Differential Diagnosis
- Osteomas: These benign tumors of bone tissue may appear similar on radiographs. Osteomas tend to present with a more irregular shape and could involve other areas of the mandible or maxilla.
- Fibrous Dysplasia: A condition characterized by abnormal bone growth, fibrous dysplasia may be confused with SPOH due to its radiopaque appearance. However, fibrous dysplasia tends to affect larger areas of bone and often shows a more “ground-glass” radiographic pattern.
- Osteomyelitis or Chronic Inflammation: Inflammatory processes that result in bone remodeling might mimic the appearance of SPOH. These conditions typically have associated soft tissue changes and clinical symptoms such as swelling or pain.
Clinical Evaluation
- Patient History: A thorough history of the patient’s dental treatment, including the presence and type of fixed prosthesis, is crucial. Any changes in occlusion or the presence of discomfort should be noted.
- Physical Examination: Palpation of the subpontic area may reveal bony changes, though this is less reliable than radiographic findings. Careful assessment of the fit of the bridge is also necessary.
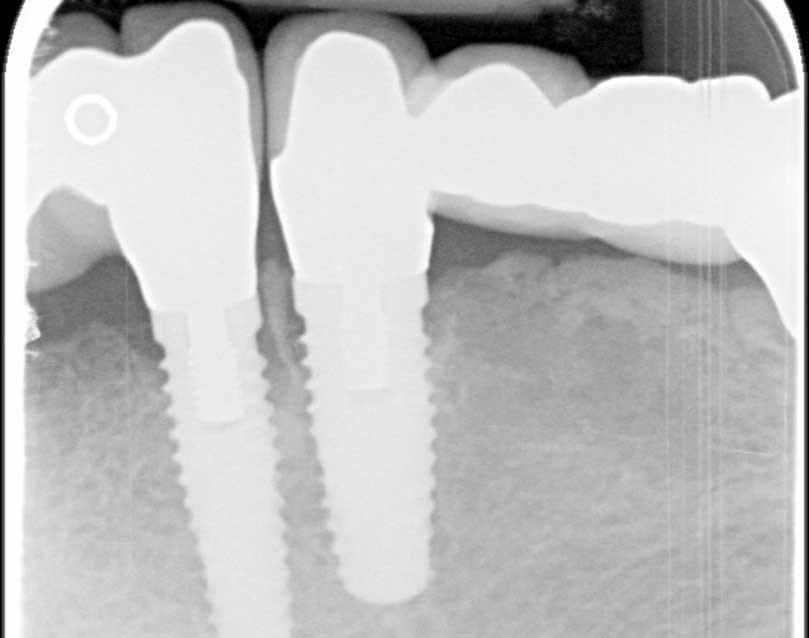
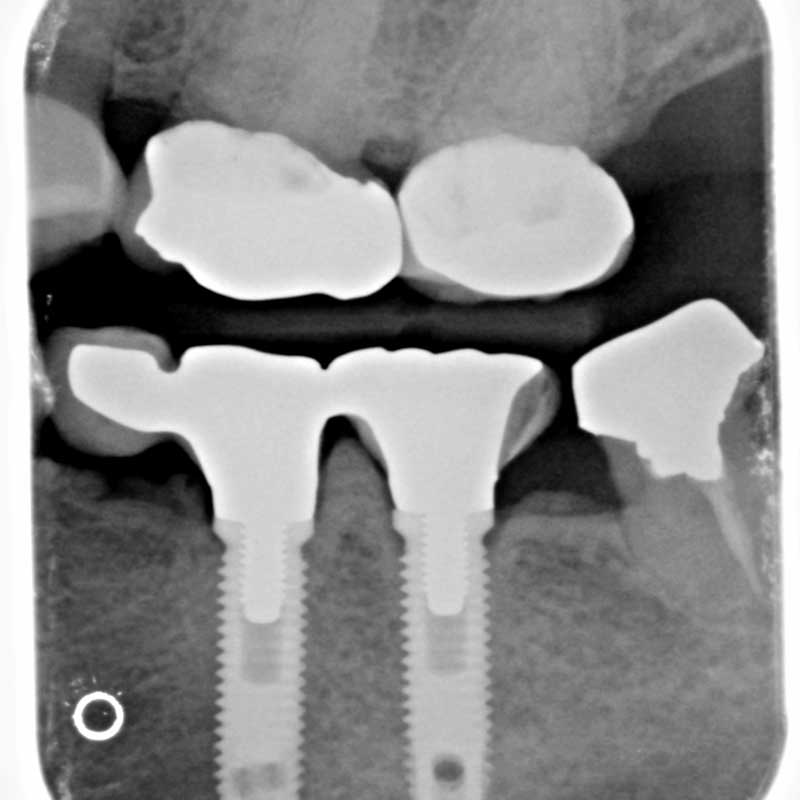
Case #2: The bone between the two closely placed implants became necrotic and painful and had to be removed.


Management and Treatment of SPOH
Management of SPOH depends on the severity of the condition and the degree to which it affects the dental prosthesis or the patient’s function. Most cases require only observation, but more severe or symptomatic cases may require intervention.
Conservative Management
- Observation: In asymptomatic cases, periodic monitoring via radiographs may be sufficient. If no significant changes are observed, the condition can be left untreated.
- Adjusting the Prosthesis: If the excessive bone growth is interfering with the function of the bridge or causing discomfort, adjustments may be made to the pontic, or the occlusion may be modified. This can alleviate any discomfort or functional problems caused by the bone growth.
Surgical Intervention
- Osseous Resection: For patients with significant bone growth that affects the fit of the bridge or causes discomfort, and no further modifications of the prosthesis can be made, surgical resection may be required. The excess bone can be removed via a simple surgical procedure, usually performed under local anesthesia.
- Prosthetic Modification: After bone resection, the pontic may need to be adjusted or replaced to ensure optimal function and esthetics. A new impression of the edentulous space may be necessary for the creation of a new or adjusted prosthesis.
Prevention
- Pontic Design: Careful attention to the design and fit of the pontic is essential. It should be contoured to minimize pressure on the alveolar ridge, and excessive bulk should be avoided.
- Oral Hygiene and Maintenance: Regular hygiene practices, including flossing around and under the pontic, are critical to preventing plaque accumulation and irritation. Professional oral prophylaxis and follow-up visits are also recommended.
- Functional Analysis: Ensuring proper occlusion and the correct distribution of masticatory forces can help reduce the risk of excessive bone formation. If occlusal discrepancies are noted, these should be corrected promptly to avoid exacerbating the condition.
- Patient Education: If we accept excessive occlusal loading to be an etiology we can educate our patients of the importance of teeth not touching unless eating. This is a surprise to many patients, but getting them to stop with the clenching and bruxism, as you know, is not an easy task and most of them when not cease this parafunctional habit.
Conclusion
Subpontic osseous hyperplasia, while not common, is an important condition for dental practitioners to recognize and understand. Its benign nature often allows for conservative management, but in cases where bone growth interferes with function or the fit of the prosthesis, intervention may be necessary. Clinicians should remain vigilant in the diagnosis of SPOH, particularly in patients with fixed partial dentures, and take proactive steps to minimize the risk through careful design, maintenance, and follow-up care. By understanding the pathophysiology, recognizing early signs, and implementing effective preventive strategies, dental professionals can ensure the long-term success of their restorative treatments and improve patient outcomes. Given the options of either losing bone or growing bone, I think we would all choose to grow bone, and this is something I do share with patients that have problems with SPOH. It is much more predictable in the management of this condition than the management of lost bone around either dental implants or teeth. We can always remove prosthetic material or bone, but getting lost bone back, especially vertical height, is not always predictable and often not possible. I have documentation of several of these cases and one thing that I did not note being discussed in the available literature is genetic pre-disposition. It is worth noting that case #2 and case #3 presented here are sisters.

Comments closed
No comments. Leave first!